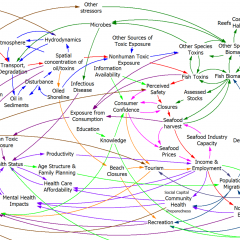
A couple weeks ago I wrote about the perceptual challenges of managing thyroid stimulating hormone (TSH), which has an exponential response to the circulating thyroid hormones (T3 & T4) you’d actually like to control.
Another facet of the thyroid control problem is noise. Generally, uncertainty in measurements is not made available to users. For example, the lab results reported by MyChart have no confidence bounds: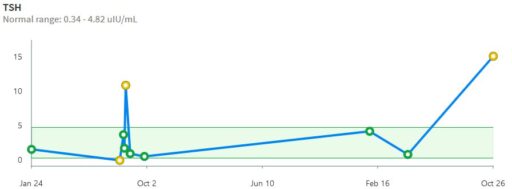
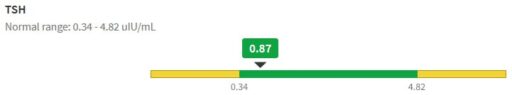 If you start looking for information on these tests, you’ll usually find precision estimates that sound pretty good – typically 5 to 7% error. (Example.) However, this understates the severity of the problem.
If you start looking for information on these tests, you’ll usually find precision estimates that sound pretty good – typically 5 to 7% error. (Example.) However, this understates the severity of the problem.
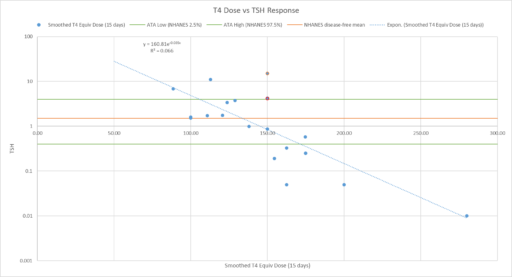
It’s well known that individual variation in the TSH<->T3,T4 setpoint is large, and the ATA guidelines mention this, if you read the detailed discussion. However, this is presented as a reason for the superiority of TSH measurements, “The logarithmic relationship between TSH and thyroid hormone bestows sensitivity: even if circulating T3 and T4 are in the normal range, it cannot be assumed that the subject is euthyroid. The interindividual ranges for T3 and T4 are much broader than the individual variance (369), such that measuring T3 and T4 is a suboptimal way to assess thyroid status.” The control implications of variation over time within an individual are not mentioned.
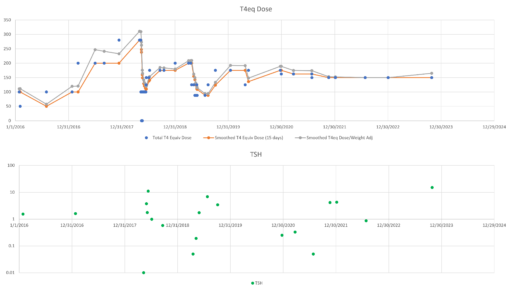
The issue we face in our N=1 sample is unexplained longitudinal variation around the setpoint. In our data, this is HUGE. At a given dose, even during a long period of stability, variation in TSH is not 10%; it’s a factor of 10.
Now consider the problem facing a doc trying to titrate your dose in a 30-minute visit. They tested your TSH, and it’s 4, or .4, right at the high or low end o the recommended range. Should they adjust the dose? (The doc’s problem is actually harder than the data presented above suggests, because they never see this much data – changes in providers, labs and systems truncate the available information to just a few points.) In our experience, 3 out of 5 doctors do change the dose, even though the confidence bounds on these measurements are probably big enough to sail the Exxon Valdez through.
There is at last a paper that tackles this issue:
Individuals exhibit fluctuations in the concentration of serum thyroid-stimulating hormone (TSH) over time. The scale of these variations ranges from minutes to hours, and from months to years. The main factors contributing to the observed within-person fluctuations in serum TSH comprise pulsatile secretion, circadian rhythm, seasonality, and ageing.
I think the right response is actually the byline of this blog: don’t just do something, stand there! If one measurement potentially has enormous variation, the first thing you should probably do is leave the dose alone and retest after a modest time. On several occasions, we have literally begged for such a retest, and been denied.
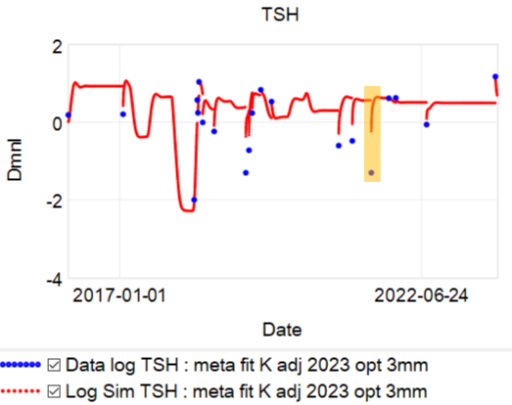
The consequence of test aversion is that we have only 20 data points over 8 years, and almost none in close proximity to one another. That makes it impossible to determine whether the variation we’re seeing is measurement error (blood draw or lab methods), fast driving noise (circadian effects), or slow trends (e.g., seasonal). I’ve been fitting models to the data for several years, but this sparsity and uncertainty gives the model fits. Here’s an example:
At the highlighted point (and half a dozen others), the model finds the data completely inexplicable. The Kalman filter moves the model dramatically towards the data (the downward spike in the red curve), but only about halfway, because the estimate yields both high measurement error and high driving noise in TSH. Because the next measurement doesn’t occur for 4 months, there’s no way to sort out which is which.
This extreme noise, plus nonlinearity previously mentioned, is really a perfect setup for errors in dose management. I’ll describe one or two in a future post.